Finding a Cheap Mental Health Billing Company in South Carolina Without Sacrificing Quality
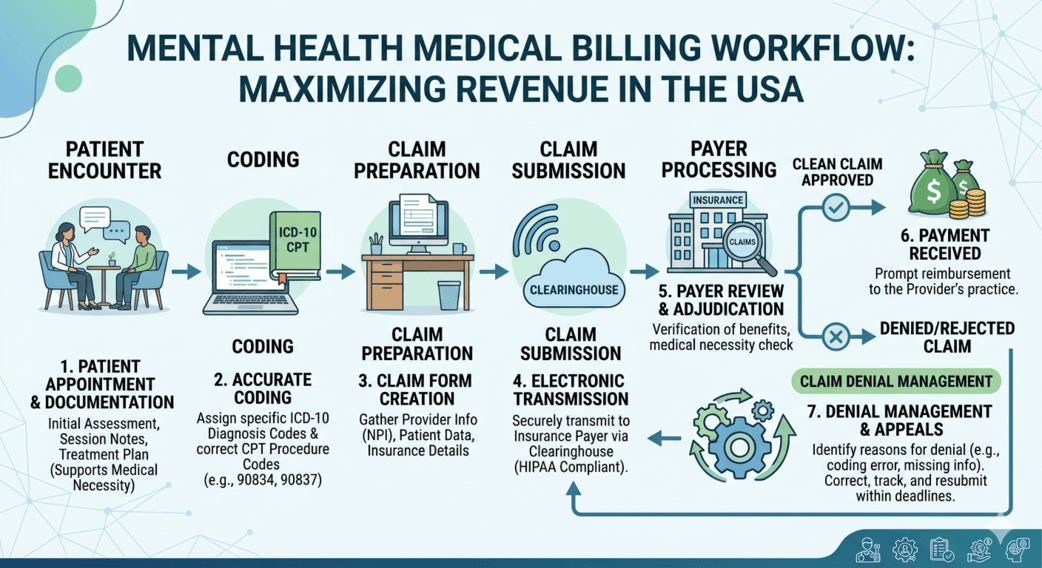
Mental health practices across South Carolina are under more pressure than ever. Therapists are managing rising patient demand, stricter payer requirements, changing telehealth regulations, and an endless stream of documentation. At the same time, reimbursement delays and denied claims continue to eat into already limited margins.
For many providers, hiring an in-house billing team simply doesn’t make financial sense anymore. Salaries, training, software subscriptions, compliance oversight, and staff turnover can quickly turn billing into one of the most expensive operational burdens in a practice.
That’s why more therapists, psychologists, psychiatrists, and behavioral health clinics are searching for a cheap mental health billing company South Carolina practices can actually rely on. The challenge, however, is finding affordability without creating even bigger problems through poor claim management or coding mistakes.
A low-cost service that mishandles claims can ultimately cost far more than it saves.
The good news is that there are specialized mental health billing companies designed specifically to help behavioral health providers reduce administrative stress while improving collections and compliance. The key is knowing what to look for and what to avoid.
Why Mental Health Billing Is More Complicated Than General Medical Billing
Mental health billing operates differently from many other healthcare specialties. Reimbursement rules vary widely between payers, session lengths differ from patient to patient, and documentation standards can become highly specific depending on diagnosis and treatment type.
A therapist in Columbia, for example, may bill individual psychotherapy sessions, family counseling, telehealth appointments, and medication management services within the same week. Each service can have different coding requirements, authorization rules, and payer expectations.
This complexity creates several common issues:
- Claims denied due to incorrect CPT or ICD-10 coding
- Missed prior authorizations
- Incomplete therapy documentation
- Telehealth billing confusion
- Delayed reimbursements
- Underpayments from insurance carriers
These problems explain why many providers eventually seek outsourced mental health billing support rather than trying to manage everything internally.
The Hidden Cost of “Cheap” Billing Services
Price matters. But in healthcare billing, the cheapest option is not always the most affordable in the long run.
Some low-cost billing vendors operate with minimal behavioral health expertise. They may process claims quickly but fail to understand nuances specific to mental health reimbursement. That can lead to recurring denials, compliance concerns, and cash flow instability.
Imagine a small therapy group in Charleston outsourcing billing to a generic medical billing provider. Initially, the monthly cost appears attractive. But within three months, the practice notices increasing denials tied to psychotherapy time-based coding errors and incomplete modifier usage for telehealth claims.
The result?
The practice spends additional hours correcting errors, appealing denials, and communicating with payers. Revenue slows down, administrative frustration increases, and the original “savings” disappear.
A qualified mental health billing and coding company should reduce work—not create more of it.
What South Carolina Mental Health Providers Should Actually Look For
Choosing a billing partner requires more than comparing prices on a website. Behavioral health practices need a provider that understands both operational efficiency and payer-specific requirements.
Specialization in Behavioral Health
Not all billing teams understand psychotherapy billing rules, mental health documentation requirements, or behavioral health coding updates.
A dedicated mental health billing agency typically has stronger expertise in:
- CPT codes for therapy sessions
- Telepsychiatry billing
- Substance abuse treatment claims
- Authorization management
- Medicaid behavioral health rules
- Insurance credentialing for therapists
Specialization often translates into fewer denials and faster reimbursement cycles.
Transparent Pricing Structure
Some companies advertise low rates but add hidden fees for credentialing, denial management, eligibility verification, or reporting.
Before signing any agreement, practices should ask:
- Is pricing percentage-based or flat-rate?
- Are there setup costs?
- Is denial management included?
- Are software fees separate?
- Are there contract minimums?
A trustworthy provider explains costs clearly upfront.
Experience With South Carolina Payers
Regional familiarity matters more than many providers realize.
An experienced team handling billing services for mental health providers in South Carolina is more likely to understand payer trends involving:
- BlueCross BlueShield of South Carolina
- Medicaid managed care organizations
- Medicare behavioral health billing
- Local authorization workflows
That insight can improve claim acceptance rates significantly.
Why Outsourcing Continues to Grow in Behavioral Health
Over the last several years, mental health practices have increasingly moved toward mental health medical billing services outsourcing because staffing challenges continue to worsen.
Hiring and retaining experienced billing staff has become difficult for many clinics. Even when practices find qualified employees, ongoing training and payer updates require constant oversight.
Outsourcing provides a different model.
Instead of maintaining an internal department, providers work with specialized billing teams that already have:
- Certified coders
- Billing software systems
- Compliance knowledge
- Claims follow-up specialists
- Denial management workflows
For smaller practices especially, outsourced mental health billing can create substantial operational relief.
A Realistic Example
Consider a two-provider counseling clinic in Greenville.
The practice previously relied on one front-desk employee to manage scheduling, insurance verification, patient calls, and billing. Claims often went out late, denials piled up, and follow-up rarely happened consistently.
After partnering with a behavioral health billing company, the clinic:
- Reduced claim submission delays
- Improved collection rates
- Shortened accounts receivable timelines
- Allowed staff to focus on patient support instead of insurance calls
The improvement wasn’t simply financial. Staff burnout decreased as well.
The Role of Technology in Modern Mental Health Billing
A strong billing partner does more than submit claims manually. Today’s successful mental health billing companies integrate technology that improves both visibility and accuracy.
Modern systems can help with:
- Real-time eligibility checks
- Electronic claim tracking
- Automated claim scrubbing
- Patient payment reminders
- Reporting dashboards
- Telehealth coding updates
These tools matter because behavioral health providers often operate with tight administrative resources. Better automation reduces human error while improving financial visibility.
However, technology alone isn’t enough.
The best outsource mental health billing and coding company combines software efficiency with human expertise. Providers still need experienced professionals reviewing denials, handling payer communication, and identifying reimbursement trends.
Common Mistakes Mental Health Practices Make With Billing
Many therapy and psychiatric practices unknowingly lose revenue due to avoidable administrative habits.
Delaying Insurance Verification
Failing to verify benefits before appointments can result in denied claims or unexpected patient balances. This issue becomes especially common with telehealth services and changing coverage rules.
Under-Coding Services
Some therapists unintentionally bill lower-level services out of caution or uncertainty. Over time, under-coding can significantly reduce revenue.
Ignoring Small Denials
A denied claim worth a small amount may seem unimportant individually. But recurring denials across hundreds of claims can create major financial losses.
Weak Documentation
Payers increasingly review therapy documentation for medical necessity. Incomplete notes can trigger audits or repayment requests.
A knowledgeable mental health billing consultant can often identify these operational gaps quickly and recommend workflow improvements.
Questions to Ask Before Hiring a Billing Company
Providers should never choose a billing vendor based solely on cost. Asking detailed questions upfront helps avoid expensive surprises later.
Important questions include:
Do You Specialize in Behavioral Health?
A company focused primarily on primary care or hospital billing may struggle with psychotherapy reimbursement rules.
How Do You Handle Denials?
Strong denial management is essential. Practices should understand how aggressively the billing team follows up on unpaid claims.
Will I Receive Reporting Access?
Financial transparency matters. Providers should have access to reports showing collections, denials, aging claims, and reimbursement trends.
What Is Your Average Claim Turnaround Time?
Slow submission processes delay revenue and disrupt cash flow.
Can You Support Growth?
As practices expand into telehealth, group therapy, or additional provider locations, billing systems should scale accordingly.
Telehealth Has Changed Mental Health Billing Permanently
Behavioral health providers across South Carolina rapidly adopted virtual care over recent years. While telehealth expanded access to care, it also introduced new billing complications.
Different payers may require:
- Specific modifiers
- Place-of-service adjustments
- Audio-only billing distinctions
- Updated authorization requirements
Practices trying to manage these updates internally often struggle to keep up.
That’s another reason mental health medical billing services outsourcing continues gaining momentum. Specialized teams monitor payer changes continuously, reducing the burden on providers.
Smaller Practices Often Benefit the Most
Large hospital systems may have internal billing infrastructure. Independent therapists and smaller behavioral health clinics usually do not.
For solo practitioners, billing can easily consume hours every week:
- Verifying insurance
- Correcting rejected claims
- Following up on unpaid balances
- Managing patient statements
- Reviewing reimbursement issues
These administrative tasks directly compete with patient care time.
Outsourced billing services for mental health therapists allow clinicians to focus more energy on treatment rather than paperwork.
In many cases, outsourcing also becomes financially smarter than maintaining internal staff salaries and training costs.
Signs It’s Time to Outsource Mental Health Billing
Some practices wait too long before seeking outside help.
A few warning signs include:
- Rising accounts receivable
- Frequent denied claims
- Delayed patient billing
- Inconsistent cash flow
- Staff burnout
- Increasing compliance concerns
- Limited reporting visibility
If any of these issues sound familiar, partnering with a top outsource mental health billing company may improve both financial performance and operational stability.
Beyond Billing: Why Integrated Revenue Support Matters
Billing alone is only one part of a successful behavioral health revenue strategy.
Many providers now prefer partners offering broader support services including:
- Insurance credentialing
- Eligibility verification
- Coding audits
- Revenue reporting
- Payment posting
- Compliance monitoring
This integrated approach helps practices maintain stronger financial performance over time.
A company providing complete medical billing and coding services can often identify operational inefficiencies that individual providers may overlook.
For example, recurring denials may not stem from coding errors at all. They could result from front-desk intake issues, expired authorizations, or incomplete documentation workflows.
Comprehensive revenue support addresses the entire reimbursement cycle rather than isolated billing tasks.
FAQs
How much do mental health billing services usually cost?
Pricing varies depending on claim volume, services included, and practice size. Most companies charge either a percentage of collections or a flat monthly fee. Lower-cost providers may appear attractive initially, but expertise and denial management quality matter just as much as price.
Is outsourcing billing safe for behavioral health practices?
Yes, as long as the billing company follows HIPAA compliance standards and uses secure systems. Reputable providers prioritize patient data protection and regulatory compliance.
Can billing companies help with therapist credentialing?
Many providers offer credentialing services alongside billing support. This can simplify enrollment with insurance payers and reduce administrative delays for growing practices.
Do outsourced billing companies work with telehealth claims?
Most experienced mental health billing companies now handle telehealth billing regularly, including modifier usage, payer updates, and virtual care reimbursement requirements.
What’s the difference between a general billing company and a mental health billing agency?
A specialized behavioral health billing company understands therapy coding, psychiatric billing requirements, documentation standards, and payer-specific mental health reimbursement rules. General billing firms may lack this expertise.
How long does it take to see financial improvement after outsourcing?
Some practices notice improvements within the first few billing cycles, especially if denial rates were previously high. Full revenue stabilization may take several months depending on claim backlogs and payer response times.
Final Thoughts
Finding a cheap mental health billing company South Carolina providers can trust is ultimately about balance. Cost matters, but accuracy, transparency, responsiveness, and behavioral health expertise matter even more.
The right billing partner should improve collections while reducing administrative stress—not simply process claims at the lowest possible rate. Practices that choose experienced behavioral health specialists often see better reimbursement consistency, stronger compliance management, and more time to focus on patient care.
As mental health practices continue evolving, comprehensive support services are becoming increasingly valuable. Providers are no longer looking only for claim submission assistance. They need dependable medical billing services, accurate medical coding services, integrated revenue cycle management, efficient credentialing services, and long-term operational guidance.
Companies like 247 Medical Billing Services are part of this shift toward more specialized behavioral healthcare support. By combining industry knowledge with tailored medical billing and coding services, they help mental health providers strengthen financial operations without losing focus on what matters most: delivering quality patient care.
- Sports
- Art
- Causes
- Crafts
- Dance
- Drinks
- Film
- Fitness
- Food
- Jogos
- Gardening
- Health
- Início
- Literature
- Music
- Networking
- Outro
- Party
- Shopping
- Theater
- Wellness


