Mental Health Insurance Billing in the USA: Complete Guide to Claims, Coding, and Reimbursement
Mental health services have become an essential part of modern healthcare in the United States. Therapists, psychologists, psychiatrists, and behavioral health clinics help millions of patients every year. However, behind every successful treatment plan lies a complex administrative process known as mental health insurance billing.
Unlike many other medical specialties, behavioral health billing involves unique coding rules, strict payer requirements, and frequent policy updates. Small documentation errors, incorrect codes, or missing authorizations can quickly lead to claim denials and delayed payments.
For mental health providers, understanding how mental health insurance billing works is critical for maintaining steady revenue and focusing on patient care rather than administrative challenges.
This guide explains how mental health billing works in the USA, the common challenges providers face, and why many practices rely on specialized billing support to manage the process efficiently.
Introduction
Mental health insurance billing is different from general medical billing in several ways. Providers must follow specific insurance policies, therapy session coding standards, and payer guidelines.
Key reasons mental health billing requires specialized expertise include:
• Complex therapy CPT codes and documentation rules
• Strict payer requirements for behavioral health services
• Pre-authorization and session limitations
• High denial rates due to coding or eligibility errors
• Constant regulatory changes in mental health coverage
Because of these complexities, many clinics rely on a mental health billing specialist or partner with professional mental health billing services to ensure accurate claims and faster reimbursements.
Understanding Mental Health Insurance Billing
Mental health insurance billing refers to the process of submitting therapy and psychiatric service claims to insurance companies for reimbursement. This process includes verifying patient benefits, coding services correctly, submitting claims, and managing payment follow-ups.
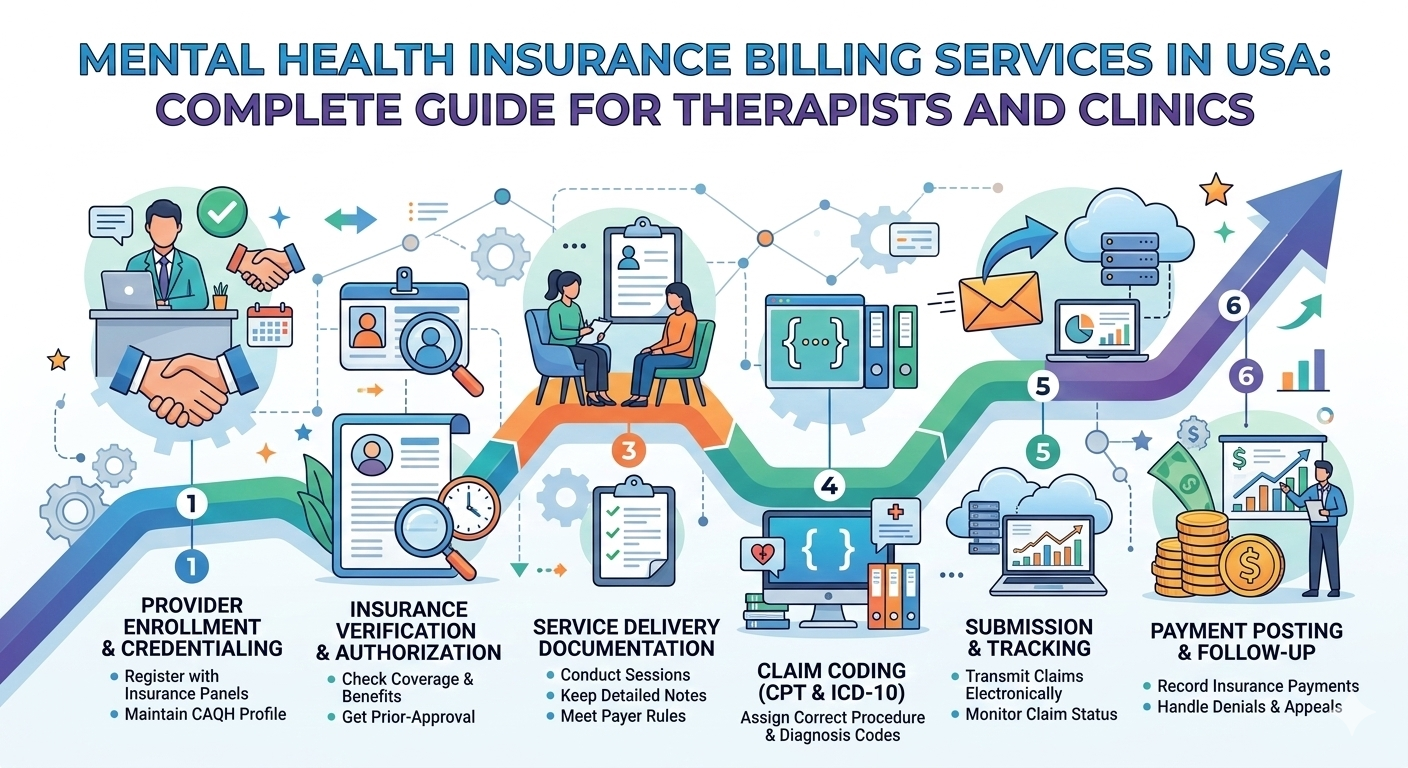
The billing process usually involves several steps:
Patient Insurance Verification
Before a therapy session begins, the billing team must confirm insurance coverage. Verification ensures that the patient’s plan covers behavioral health services and identifies co-pays, deductibles, and session limits.
Pre-Authorization Requirements
Some insurers require prior authorization for therapy or psychiatric treatments. Without authorization, claims may be denied even if the service was medically necessary.
Accurate Medical Coding
Correct CPT and diagnosis codes are essential in mental health medical billing services. Coding must accurately reflect the type of therapy, session duration, and diagnosis.
Claim Submission
Once coding is complete, the claim is submitted electronically to the payer. A professional mental health billing company ensures the claim meets payer requirements before submission.
Payment Posting and Follow-Up
After submission, insurers process the claim. Billing teams track claim status, post payments, and resolve denials if they occur.
These steps highlight why many providers work with a mental health billing services company that specializes in behavioral health claims.
Common Challenges in Mental Health Billing
Mental health providers often face several billing challenges that can affect revenue and administrative workload.
Frequent Claim Denials
Insurance companies carefully review mental health claims. Missing documentation, incorrect modifiers, or coding errors can quickly lead to denials.
Complex Coding Requirements
Behavioral health services include multiple CPT codes for psychotherapy sessions, family therapy, psychiatric evaluations, and medication management. Mental health billing and coding company experts ensure these codes are used correctly.
Insurance Policy Variations
Different insurance providers have different rules for therapy coverage. A mental health billing consultant understands these payer-specific policies.
Session Limits and Authorization Rules
Many insurance plans limit the number of therapy sessions per year. Billing teams must track usage to prevent claim rejections.
Administrative Burden on Therapists
When therapists handle billing themselves, it reduces the time available for patient care. Billing services for mental health therapists help reduce this workload and improve efficiency.
Role of a Mental Health Billing Specialist
A mental health billing specialist plays an important role in ensuring accurate claims and proper reimbursement. Their responsibilities extend beyond basic billing tasks.
Key responsibilities typically include:
• Insurance eligibility verification
• CPT and ICD coding for behavioral health services
• Claim submission and tracking
• Payment reconciliation
• Denial management and appeals
• Compliance with payer regulations
Many healthcare organizations rely on mental health billing specialist companies that focus entirely on behavioral health billing processes.
Benefits of Outsourcing Mental Health Billing
Because of the complexity of insurance rules and coding requirements, many practices choose to outsource mental health billing services instead of handling billing internally.
Outsourced billing offers several advantages.
Improved Revenue Management
Experienced billing teams reduce errors and improve claim acceptance rates. This ensures consistent cash flow for the practice.
Reduced Administrative Work
Outsourced mental health billing allows providers to focus on therapy sessions rather than paperwork.
Expert Coding Knowledge
A top outsource mental health billing company stays updated on payer guidelines, CPT code updates, and regulatory changes.
Faster Claims Processing
Professional billing teams submit clean claims quickly, which helps accelerate reimbursement timelines.
Lower Operational Costs
Hiring an internal billing team can be expensive. Mental health medical billing services outsourcing allows clinics to access expert services without the cost of in-house staff.
These advantages explain why many providers search for the best outsource mental health billing and coding company to manage their revenue cycle.
Choosing the Right Mental Health Billing Company
Selecting the right billing partner is an important decision for any behavioral health practice.
A reliable mental health billing provider should offer:
Industry-Specific Experience
The company should have experience in behavioral & mental health billing services rather than general healthcare billing alone.
Transparent Reporting
Providers should receive regular reports on claim status, reimbursements, and denial trends.
Certified Coding Experts
A strong mental health billing company employs certified coders who understand psychotherapy coding and insurance policies.
Technology Integration
Modern billing systems allow seamless integration with electronic health records and practice management software.
Dedicated Support
A professional mental health billing company typically provides dedicated account managers to address provider concerns.
Practices often evaluate several mental health billing companies before selecting the best mental health billing services company that aligns with their needs.
Services Offered by Mental Health Billing Agencies
A full-service mental health billing agency usually provides comprehensive support for the entire billing cycle.
Common services include:
Insurance verification and eligibility checks
CPT and ICD coding for behavioral health services
Electronic claim submission
Denial management and appeals
Payment posting and reconciliation
Accounts receivable management
Compliance monitoring
These services help billing companies for mental health providers maintain consistent revenue while minimizing administrative work.
Some clinics also rely on a mental health billing consultant to review existing billing systems and identify areas for improvement.
Why Mental Health Billing Requires Specialized Expertise
Mental health billing differs from standard medical billing due to its documentation requirements, therapy coding standards, and payer rules.
For example:
Psychotherapy sessions are coded based on time duration
Family therapy sessions have separate coding rules
Telehealth mental health services require special modifiers
Insurance providers often require detailed treatment documentation
Because of these complexities, many clinics partner with the best mental health billing agency or a top mental health billing company to ensure accurate claim management.
Professional billing agencies also help practices adapt to policy changes and maintain compliance with healthcare regulations.
Technology and Modern Mental Health Billing Solutions
Technology has significantly improved billing efficiency in behavioral healthcare.
A modern mental health medical billing solution often includes:
Automated claim scrubbing tools
Electronic eligibility verification
Integrated coding support
Real-time claim tracking
Analytics and reporting dashboards
These technologies help reduce billing errors and improve reimbursement timelines.
When combined with outsourcing mental health billing and coding expertise, these tools allow practices to streamline their revenue cycle operations.
Supporting Mental Health Providers with Complete Billing Services
Mental health providers need reliable billing processes to maintain financial stability while delivering quality patient care.
Professional billing partners offer structured solutions that include billing services for mental health providers, compliance support, and ongoing revenue monitoring.
Many practices now rely on a mental health billing services agency that specializes in behavioral health revenue cycle management.
Companies like 247 Medical Billing Services support healthcare providers through comprehensive services including medical billing services, medical coding services, medical billing and coding services, revenue cycle management, and credentialing services. These services help healthcare organizations manage administrative processes more effectively while maintaining compliance and improving reimbursement efficiency.
Conclusion
Mental health insurance billing plays a crucial role in the financial health of behavioral healthcare practices across the United States. From insurance verification and coding to claim submission and denial management, each step requires precision and expertise.
As insurance policies become more complex and documentation requirements continue to evolve, many providers find it beneficial to partner with experienced billing specialists or outsource mental health billing services.
With the right billing strategy, mental health providers can reduce administrative stress, improve reimbursement rates, and focus on what matters most: delivering quality care to patients.
Frequently Asked Questions
What is mental health insurance billing?
Mental health insurance billing is the process of submitting claims to insurance companies for therapy, psychiatric care, and behavioral health services. It involves insurance verification, coding, claim submission, and reimbursement management.
Why is mental health billing different from general medical billing?
Mental health billing involves unique CPT codes, strict documentation requirements, and therapy session time-based coding, which makes it more complex than many other medical billing specialties.
Why do providers outsource mental health billing?
Many providers outsource mental health billing to reduce administrative workload, improve claim accuracy, and ensure faster reimbursements through experienced billing specialists.
What services do mental health billing companies provide?
Mental health billing companies typically provide insurance verification, coding, claim submission, denial management, accounts receivable management, and compliance support.
How can a mental health billing specialist help providers?
A mental health billing specialist ensures that claims are coded correctly, submitted on time, and followed up with insurance companies, helping providers reduce denials and improve revenue flow.
- Sports
- Art
- Causes
- Crafts
- Dance
- Drinks
- Film
- Fitness
- Food
- Παιχνίδια
- Gardening
- Health
- Κεντρική Σελίδα
- Literature
- Music
- Networking
- άλλο
- Party
- Shopping
- Theater
- Wellness


